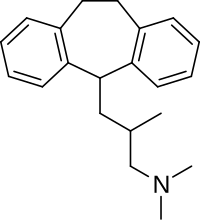
Butriptyline
 | |
| Clinical data | |
|---|---|
| Trade names | Evadyne, others |
| Other names | AY-62014[1] |
| Routes of administration | Oral |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | ?[3] |
| Protein binding | >90%[3] |
| Metabolism | Hepatic (N-demethylation) |
| Metabolites | Norbutriptyline[3] |
| Elimination half-life | 20 hours[3] |
| Identifiers | |
| |
| CAS Number |
|
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII |
|
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| Chemical and physical data | |
| Formula | C21H27N |
| Molar mass | 293.454 g·mol−1 |
| 3D model (JSmol) | |
| Chirality | Racemic mixture |
| |
| |
| | |
Butriptyline, sold under the brand name Evadyne among others, is a tricyclic antidepressant (TCA) that has been used in the United Kingdom and several other European countries for the treatment of depression but appears to no longer be marketed.[1][4][5][6][7] Along with trimipramine, iprindole, and amoxapine, it has been described as an "atypical" or "second-generation" TCA due to its relatively late introduction and atypical pharmacology.[8][9] It was very little-used compared to other TCAs, with the number of prescriptions dispensed only in the thousands.[10]
Medical uses
[edit]Butriptyline was used in the treatment of depression.[11] It was usually used at dosages of 150–300 mg/day.[12]
Side effects
[edit]Butriptyline is closely related to amitriptyline, and produces similar effects as other TCAs, but its side effects like sedation are said to be reduced in severity and it has a lower risk of interactions with other medications.[6][7][10]
Butriptyline has potent antihistamine effects, resulting in sedation and somnolence.[13] It also has potent anticholinergic effects,[14] resulting in side effects like dry mouth, constipation, urinary retention, blurred vision, and cognitive/memory impairment.[13] The drug has relatively weak effects as an alpha-1 blocker and has no effects as a norepinephrine reuptake inhibitor,[15][16] so is associated with little to no antiadrenergic and adrenergic side effects.[15][14][additional citation(s) needed]
Overdose
[edit]Pharmacology
[edit]Pharmacodynamics
[edit]| Site | Ki (nM) | Species | Ref |
|---|---|---|---|
| SERT | 1,360 4,300 10,000 (IC50) | Human Rat Rat | [16] [18] [19] |
| NET | 5,100 990 1,700 (IC50) | Human Rat Rat | [16] [18] [19] |
| DAT | 3,940 2,800 5,200 (IC50) | Human Rat Rat | [16] [18] [19] |
| 5-HT1A | 7,000 | Human | [20] |
| 5-HT2A | 380 | Human | [20] |
| 5-HT2C | ND | ND | ND |
| α1 | 570 | Human | [15] |
| α2 | 4,800 | Human | [15] |
| D2 | ND | ND | ND |
| H1 | 1.1 | Human | [15] |
| mACh | 35 | Human | [15] |
| Values are Ki (nM), unless otherwise noted. The smaller the value, the more strongly the drug binds to the site. | |||
In vitro, butriptyline is a strong antihistamine and anticholinergic, moderate 5-HT2 and α1-adrenergic receptor antagonist, and very weak or negligible monoamine reuptake inhibitor.[15][20][16][19] These actions appear to confer a profile similar to that of iprindole and trimipramine with serotonin-blocking effects as the apparent predominant mediator of mood-lifting efficacy.[21][19][18]
However, in small clinical trials, using similar doses, butriptyline was found to be similarly effective to amitriptyline and imipramine as an antidepressant, despite the fact that both of these TCAs are far stronger as both 5-HT2 antagonists and serotonin–norepinephrine reuptake inhibitors.[15][20][22] As a result, it may be that butriptyline has a different mechanism of action, or perhaps functions as a prodrug in the body to a metabolite with different pharmacodynamics.
Pharmacokinetics
[edit]Therapeutic concentrations of butriptyline are in the range of 60–280 ng/mL (204–954 nmol/L).[23] Its plasma protein binding is greater than 90%.[3]
Chemistry
[edit]Butriptyline is a tricyclic compound, specifically a dibenzocycloheptadiene, and possesses three rings fused together with a side chain attached in its chemical structure.[24] Other dibenzocycloheptadiene TCAs include amitriptyline, nortriptyline, and protriptyline.[24] Butriptyline is an analogue of amitriptyline with an isobutyl side chain instead of a propylidene side chain.[10][25] It is a tertiary amine TCA, with its side chain-demethylated metabolite norbutriptyline being a secondary amine.[26][27] Other tertiary amine TCAs include amitriptyline, imipramine, clomipramine, dosulepin (dothiepin), doxepin, and trimipramine.[28][29] The chemical name of butriptyline is 3-(10,11-dihydro-5H-dibenzo[a,d]cycloheptene-5-yl)-N,N,2-trimethylpropan-1-amine and its free base form has a chemical formula of C21H27N with a molecular weight of 293.446 g/mol.[1] The drug has been used commercially both as the free base and as the hydrochloride salt.[1][4] The CAS Registry Number of the free base is 15686-37-0 and of the hydrochloride is 5585-73-9.[1][4]
History
[edit]Butriptyline was developed by Wyeth and introduced in the United Kingdom in either 1974 or 1975.[5][30][31]
Society and culture
[edit]Generic names
[edit]Butriptyline is the English and French generic name of the drug and its INN, BAN, and DCF, while butriptyline hydrochloride is its BANM and USAN.[1][4][11] Its generic name in Latin is butriptylinum, in German is butriptylin, and in Spanish is butriptylina.[4]
Brand names
[edit]Butriptyline has been marketed under the brand names Evadene, Evadyne, Evasidol, and Centrolese.[1][4][5]
Availability
[edit]Butriptyline has been marketed in Europe, including in the United Kingdom, Belgium, Luxembourg, Austria, and Italy.[4][5]
References
[edit]- ^ a b c d e f g Elks J (14 November 2014). The Dictionary of Drugs: Chemical Data: Chemical Data, Structures and Bibliographies. Springer. pp. 201–. ISBN 978-1-4757-2085-3.
- ^ Anvisa (2023-03-31). "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 2023-04-04). Archived from the original on 2023-08-03. Retrieved 2023-08-16.
- ^ a b c d e Dörwald FZ (4 February 2013). "Dibenzazepines and Related Tricyclic Compounds". Lead Optimization for Medicinal Chemists: Pharmacokinetic Properties of Functional Groups and Organic Compounds. John Wiley & Sons. pp. 313–. ISBN 978-3-527-64565-7.
- ^ a b c d e f g Swiss Pharmaceutical Society (2000). Index Nominum 2000: International Drug Directory (Book with CD-ROM). Boca Raton: Medpharm Scientific Publishers. ISBN 3-88763-075-0. Archived from the original on 2023-01-12. Retrieved 2020-10-30.
- ^ a b c d William Andrew Publishing (22 October 2013). Pharmaceutical Manufacturing Encyclopedia. Elsevier. pp. 777–. ISBN 978-0-8155-1856-3.
- ^ a b Holenz J, Diaz JL, Buschmann H (16 April 2007). "Tricyclic and tetracyclic antidepressants". In Buschmann H (ed.). Antidepressants, Antipsychotics, Anxiolytics: From Chemistry and Pharmacology to Clinical Application. Wiley. pp. 180–. ISBN 978-3-527-31058-6.[permanent dead link]
- ^ a b Paykel ES (1992). Handbook of Affective Disorders. Guilford Press. pp. 339–. ISBN 978-0-89862-674-2.
- ^ Sharma SS, Chawala P (18 November 2009). "Drug Therapy of Affective Disorders". In Seth A (ed.). Textbook Of Pharmacology. Elsevier India. pp. 119–. ISBN 978-81-312-1158-8.
- ^ Bhattacharya A (2003). "Central Nervous System". Pharmacology (2nd ed.). Elsevier India. pp. 292–. ISBN 978-81-8147-009-6.
- ^ a b c Aronson JK (2009). Meyler's Side Effects of Psychiatric Drugs. Elsevier. pp. 7, 18, 31. ISBN 978-0-444-53266-4. Archived from the original on 2024-07-26. Retrieved 2017-08-13.
- ^ a b Morton IK, Hall JM (6 December 2012). Concise Dictionary of Pharmacological Agents: Properties and Synonyms. Springer Science & Business Media. pp. 58–. ISBN 978-94-011-4439-1.
- ^ Paykel ES (29 October 1982). "Treatment for Affective Disorders". In Wing JK, Wing L (eds.). Handbook of Psychiatry: Volume 3, Psychoses of Uncertain Aetiology. CUP Archive. pp. 167–. ISBN 978-0-521-28438-7.
- ^ a b Gillman PK (July 2007). "Tricyclic antidepressant pharmacology and therapeutic drug interactions updated". British Journal of Pharmacology. 151 (6): 737–748. doi:10.1038/sj.bjp.0707253. PMC 2014120. PMID 17471183.
- ^ a b Mumenthaler M, van Zwieten PA, Farcot JM, eds. (1990). "Reactions to Antidepressant Drugs and Lithium Salts". Treatment of Chronic Pain: Possibilities, Limitations, and Long-term Follow-up. CRC Press. pp. 114–. ISBN 978-3-7186-5027-9. Archived from the original on 2024-07-26. Retrieved 2017-08-13.
- ^ a b c d e f g h Richelson E, Nelson A (July 1984). "Antagonism by antidepressants of neurotransmitter receptors of normal human brain in vitro". The Journal of Pharmacology and Experimental Therapeutics. 230 (1): 94–102. PMID 6086881.
- ^ a b c d e Tatsumi M, Groshan K, Blakely RD, Richelson E (December 1997). "Pharmacological profile of antidepressants and related compounds at human monoamine transporters". European Journal of Pharmacology. 340 (2–3): 249–258. doi:10.1016/s0014-2999(97)01393-9. PMID 9537821.
- ^ Roth BL, Driscol J. "PDSP Ki Database". Psychoactive Drug Screening Program (PDSP). University of North Carolina at Chapel Hill and the United States National Institute of Mental Health. Archived from the original on 2 December 2023. Retrieved 14 August 2017.
- ^ a b c d Richelson E, Pfenning M (September 1984). "Blockade by antidepressants and related compounds of biogenic amine uptake into rat brain synaptosomes: most antidepressants selectively block norepinephrine uptake". European Journal of Pharmacology. 104 (3–4): 277–286. doi:10.1016/0014-2999(84)90403-5. PMID 6499924.
- ^ a b c d e Randrup A, Braestrup C (August 1977). "Uptake inhibition of biogenic amines by newer antidepressant drugs: relevance to the dopamine hypothesis of depression". Psychopharmacology. 53 (3): 309–314. doi:10.1007/BF00492370. PMID 408861. S2CID 8183053.
- ^ a b c d Wander TJ, Nelson A, Okazaki H, Richelson E (December 1986). "Antagonism by antidepressants of serotonin S1 and S2 receptors of normal human brain in vitro". European Journal of Pharmacology. 132 (2–3): 115–121. doi:10.1016/0014-2999(86)90596-0. PMID 3816971.
- ^ Jaramillo J, Greenberg R (February 1975). "Comparative pharmacological studies on butriptyline and some related standard tricyclic antidepressants". Canadian Journal of Physiology and Pharmacology. 53 (1): 104–112. doi:10.1139/y75-014. PMID 166748.
- ^ Stuart S (22 October 2013). "Tricyclic Antidepressants". Drugs in Psychiatric Practice. Elsevier. pp. 194–. ISBN 978-1-4831-9193-5. Archived from the original on 26 July 2024. Retrieved 13 August 2017.
- ^ Smith RN (6 December 2012). "Radioimmunoassay of Drugs in Body Fluids in a Forensic Context". In Maehly A, Williams RL (eds.). Forensic Science Progress. Springer Science & Business Media. pp. 24–. ISBN 978-3-642-73058-0.
- ^ a b Ritsner MS (15 February 2013). "Appendix 2: List of Psychotropic Medications". Polypharmacy in Psychiatry Practice, Volume I: Multiple Medication Use Strategies. Springer Science & Business Media. pp. 270–271. ISBN 978-94-007-5805-6.
- ^ Zavod RM, Knittel JJ (24 January 2012). "Drug Design and Relationship of Functional Groups to Pharmacological Activity". In Lemke TL, Williams DA (eds.). Foye's Principles of Medicinal Chemistry. Lippincott Williams & Wilkins. pp. 604–. ISBN 978-1-60913-345-0. Archived from the original on 12 January 2023. Retrieved 13 August 2017.
- ^ Dawkins K, Manji HK, Potter WZ (20 September 1994). "Pharmacodynamics of Antidepressants". In Cutler NR, Sramek JJ, Narang PK (eds.). Pharmacodynamics and Drug Development: Perspectives in Clinical Pharmacology. John Wiley & Sons. pp. 160–. ISBN 978-0-471-95052-3.
- ^ Baumann P, Hiemke C (23 February 2012). "Central Nervous System Drugs". In Anzenbacher P, Zanger UM (eds.). Metabolism of Drugs and Other Xenobiotics. John Wiley & Sons. pp. 302–. ISBN 978-3-527-64632-6.
- ^ Anthony PK (2002). "Drugs Used in the Therapy of Depression". Pharmacology Secrets. Elsevier Health Sciences. pp. 39–. ISBN 1-56053-470-2. Archived from the original on 2023-01-10. Retrieved 2017-08-16.
- ^ Cowen P, Harrison P, Burns T (9 August 2012). "Drugs and Other Physical Treatments". Shorter Oxford Textbook of Psychiatry. OUP Oxford. pp. 532–. ISBN 978-0-19-162675-3. Archived from the original on 10 January 2023. Retrieved 16 August 2017.
- ^ Ghose K (11 November 2013). "Side-effects of tricyclic and related antidepressants". In Ghose K (ed.). Antidepressants for Elderly People. Springer. pp. 182–. ISBN 978-1-4899-3436-9. Archived from the original on 14 January 2023. Retrieved 13 August 2017.
- ^ Dawson AH (2004). "Cyclic Antidepressant Drugs". In Dart RC (ed.). Medical Toxicology. Lippincott Williams & Wilkins. pp. 836–. ISBN 978-0-7817-2845-4.


 French
French Deutsch
Deutsch